
Technical Information





-
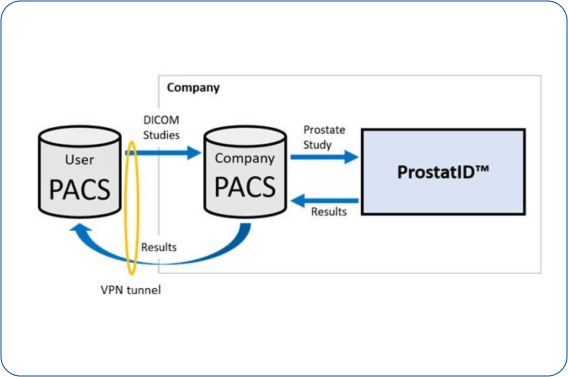
- Predicate Device: TransparaM by Screen Point Medical B.V.
- FDA-cleared software product for diagnosis of breast cancer lesions
- same intended use as ProstatID:
- “Radiological computer-assisted detectionand diagnostic (CAD) software for lesions suspicious for cancer”
- allows for a 510(k) approval process
- FDA 510(k) Submission
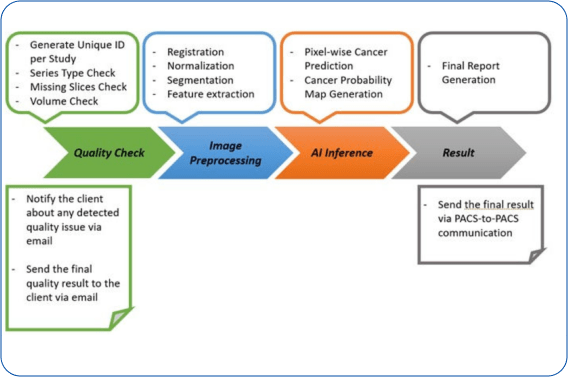
- Standalone Performance Assessment
- The developed ProstatID software was tested internally to evaluate the correlation of its outputs to a reference standard.
- Tested on 150 patient cases set aside prior to algorithm training.
- Clinical Performance Assessment
- Evaluated the effect of using the ProstatID software in the clinical setting.
- Tested on a separate set of 150 patient cases selected prior to training.
- Recruited 12 physicians to participate:
- 1st Read: current standard of care without ProstatID
- Tested on a separate set of 150 patient cases selected prior to training.
- 2nd Read: current standard of care with ProstatID
- Standalone Performance Assessment
- Predicate Device: TransparaM by Screen Point Medical B.V.
-
- Standalone Performance Assessment
- ROC analysis of ProstatID index value and true outcomes
- 3mm regions of entire prostate region analyzed
- 150 patient cases → 77 benign, 73 cancer
- Results: overall AUC = 0.852 [0.816, 0.888]
- also broken down into different MR field strength
- Standalone Performance Assessment
- Multiple reader, multiple case (MRMC) study design
- 12 physicians reading 150 cases to achieve statistical power of 0.80
- 150 retrospective patient cases → 80 benign, 70 cancer
- Readers instructed to give each detected lesion a score 1-5 (PI-RADS v2)
- Results: average change in AUC = +0.061 [0.016, 0.105] (p = 0.0097)
when using ProstatID
- Standalone Performance Assessment
-
-
-
- Improved detection accuracy by 27.8% using FROC analyses
- Decreased False Positive (biopsies) by 36%
-
-




